Elderly Onset Rheumatoid Arthritis: What to Know
Category:

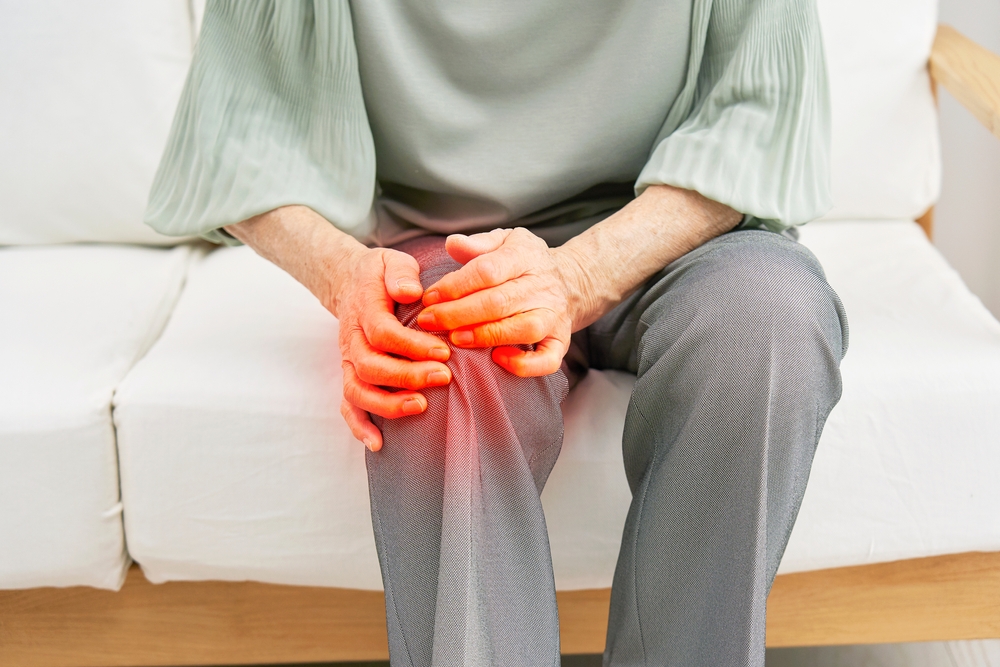
Rheumatoid arthritis (RA) is an inflammatory disease that causes swelling, pain, stiffness, discomfort, and loss of function in the joints of the body. Rheumatoid arthritis is more prevalent in women, and it is often diagnosed between the ages of 30-60.
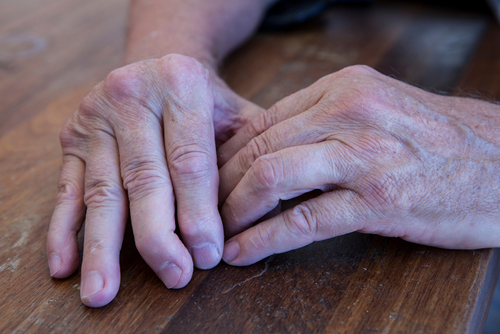
The condition tends to present itself symmetrically, which means the coordinating joints on both sides of the body are affected. As the tissue lining surrounding the joints becomes thickened, severe pain and swelling occur. Over a long period of time, the inflammation can cause loss of bone mass and joint deformity.
Rheumatoid arthritis in elderly adults is commonly referred to as elderly onset rheumatoid arthritis or EORA. Having a relative with rheumatoid arthritis increases the odds of developing the condition.
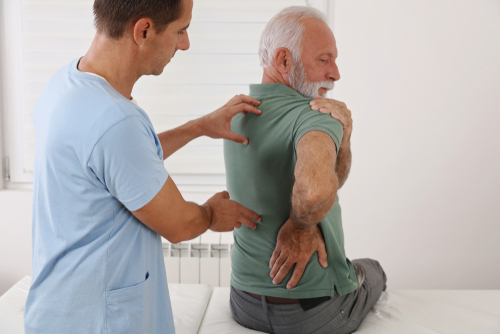
Elderly onset rheumatoid arthritis affects men and women more equally as they age, and it often seems to affect large joints, such as the shoulders.
Elderly onset rheumatoid arthritis symptoms:
- Pain and tenderness in the affected joints.
- Swelling and aching in more than one joint.
- Stiffness, especially in the early morning.
- Low-grade fever with no other explanation.
- Weakness and loss of stamina.
- Fatigue that is not relieved by resting.
- Unexplained weight loss that is not intentional.
- Loss of function and mobility due to pain and discomfort.
If you think you might be a victim of rheumatoid arthritis, the first step is to make an appointment with your doctor to get a proper diagnosis. Rheumatoid arthritis is often underdiagnosed in the elderly because it sometimes mimics other illnesses.
How is an elderly onset rheumatoid arthritis diagnosis determined?
Your doctor will review your complete medical history, ask questions about your symptoms, and perform a physical exam of the affected joints.
Rheumatoid arthritis is an autoimmune disease, so bloodwork will be a necessary component in the diagnostic procedure. Your blood will be tested for biomarkers of autoimmunity such as rheumatoid factor and anticitrullinated protein antibody.
Additionally, your physician may recommend PET or CT scans for further evaluation.
Elderly onset rheumatoid arthritis treatment:
- Non-steroidal anti-inflammatory (NSAID) drugs such as Ibuprofen can be used to reduce pain and swelling.
- Corticosteroid drugs, such as prednisone are prescribed for quick relief of symptoms, but the side effects and risks must be closely monitored when these drugs are prescribed.
- Methotrexate is a drug used for long-term treatment and relief of the symptoms of rheumatoid arthritis. This drug can be taken along with a steroid or NSAID. Although most people tolerate it very well, people with lung or kidney disease must be closely monitored if methotrexate is prescribed.
Download Our Joint Pain Remedy Guide
The management of rheumatoid arthritis in elderly people can lead to improved quality of life if the patient adheres to the following recommendations:
- Get plenty of sleep. Sleep deprivation can worsen the symptoms of rheumatoid arthritis.
- Exercise as much as possible. Movement helps to maintain joint mobility. Exercise is also a mood elevator, and it can help you to sleep better at night.
- Eat a healthy diet, maintain a healthy weight, and eliminate foods that cause inflammation such as fast food, sugar, soft drinks, trans fats, refined carbohydrates, alcohol, and processed meats.
- Be aware of the side effects of rheumatoid arthritis medications and report them to your doctor immediately.
Partnering with your medical professional is the best way to get optimal relief from the pain and discomfort of elderly onset rheumatoid arthritis. With the guidance of your physician, effective medicinal treatment for your specific case, and self-determination, you should be able to live your best life as you develop a plan of care that works best for you.
Subscribe
Date: November 2, 2021
Category: